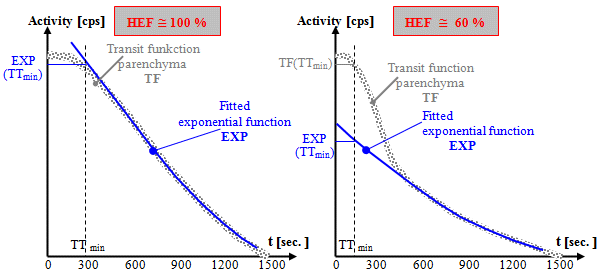
Calculation of the hepatic extraction fraction HEP based on the analysis of the deconvolution transit curve of the parenchyma.
Back: List of complex programs
3.10. Comprehensive
evaluation of a dynamic study of the liver and
bile ducts
(cholescintigraphy)
Dynamic liver scintigraphy (cholescintigraphy) is used for qualitative and quantitative evaluation of liver function and bile duct kinetics . A comprehensive mathematical evaluation of this dynamic study includes the following main points: *)
*) Dynamic scintigraphy of the liver with its character is very similar to dynamic sequential scintigraphy of the kidneys, so that a number of similar procedures are used in its computer evaluation. Therefore, before reading this chapter, we recommend that you first study chapter 3.4. on computer evaluation of dynamic renal scintigraphy, where the relevant methods and procedures are described in more detail. This also applies to the sample the method of determining the clearance, that the dynamic scintigraphy liver practically not used.
Data storage
We perform the examination lying down, while the scintillation camera detector equipped with a corresponding collimator is directed at the patient's abdominal cavity. Prepare the appropriate 99m Tc-HIDA or EHIDA radio indicator with an activity of approx. 100 MBq in the syringe . We specify the position of the patient under the detector by applying a pointer or a syringe with prepared activity above the proc before application. xyphoides and as it moves along the right rib arch, make sure that the trace of the poi n teru is displayed on the screen of the monitor or persistent oscilloscope in the right middle part of the field of view (so that the liver is in the upper left part of the field of view).
We then quickly apply the indicator *) (we recommend rinsing the syringe with saline) and start saving the dynamic scintigraphic study.
Recommended storage mode:
matrix 64x64, preset 180 frames after 20 sec. .
If the retention of a radiolabel in the gallbladder is visible on the screen after about 30 minutes , it is recommended that a cholekinetic stimulus be administered (preferably cholecystokinin, if not available, eg chocolate) and continue to study until the 90th minute, if possible. during the evaluation they could assess the response of the gallbladder to the cholekinetic stimulus. Only in the case of a quick passage is it enough to save the study for about 60 minutes. With the retention of the radioinducer, we usually store a still image after 3 hours, on which we assess whether the radioindicator still gets into the intestinal tract and what part.
Study evaluation
After invoking a scintigraphic study in the basic OSTNUCLINE system, we will launch a comprehensive HEPDYN program - a dynamic study of the liver .
Visual evaluation of sequential images
First, a series of appropriately absorbed images (together with the values ??of the respective time intervals) is created on the screen, capturing the distribution and course of accumulation of the radioindicator in the liver and its excretion by the biliary tract into the intestinal tract. According to these images, a preliminary verbal evaluation can be preselected , both as an implicit standard formulation of a normal evaluation with the gallbladder, e.g.
Following intravenous
administration of the radioindicator,
livers of the usual shape and size are
imaged in a timely manner
. Hepatic parenchyma without apparent focal changes. This is followed by
filling of the intrahepatic bile ducts
with a smooth outflow through the ductus choledochus to the
intest. tract.
Conclusion:
Visual evaluation of sequential scintigrams as well as
quantitative analysis of
liver curves indicate good hepatocellular function, rapid
transit through the liver parenchyma and free drainage of the
bile system. ,
Or without gallbladder, e.g.
Following intravenous
administration of the radioindicator,
livers of appropriate size and shape are imaged in a timely
manner . The liver parenchyma does not show
focal changes. Bile ducts can be differentiated from ... min.,
From ... min. the gallbladder begins to fill. V ...
min. a
cholekinetic stimulus
was administered . In the
next course, we observe a rapid
passage of
the radioindicator through the biliary system with a smooth
outflow through the ductus choledochus into the intest. tract.
Conclusion:
Visual evaluation sequence and scintigrams quantitative
An analysis of liver
curves are good indicative of hepatocellular
function, rapid transit liver parenchyma and the free passage of
the biliary system, without signs of biliary obstruction.
The gallbladder has a good filling and evacuation function. ,
so non-standard text . The series about brazi together with the verbal evaluation can be printed for documentation, but there is usually no reason to do so - a final protocol will suffice.
Designation of areas of interest and creation of curves
Then the following areas of interest are marked:
Bloodstream ......... ........ ROI 1
Whole liver ........................ ROI 2
Hepatic parenchym .......... ROI 3
Ductus choledochus ....... ROI 4
Intestinal tract .............. ROI 5
Gallbladder .......
................... ROI 6
(if displayed)
Stomach
..................... .. ... ROI 7 (only in case of duodenal-gastric reflux)
For the area of interest of the blood pool, we will use the images immediately after the arrival of the activity. As ROI 1, we mark the perfused structures high enough above the liver here, it is desirable to use the precordium area if it is in the field of view. The area of ??interest of the whole liver is marked in the following images of the secretory phase. After another odkrokování images mark the liver parenchyma ROI - due to the normalization of the curves enough to indicate a typical piece parenchyma, Best s pe outer part of the intrahepatic biliary unaffected. We also mark the area of interest of the ductus choledochus and mark the area of intest on sufficiently late images. tract. As ROI 6, we mark the gallbladder area, if this is displayed. If during the study, the radioindicator also appeared in the stomach (due to duodenal-gastric reflux), we mark the stomach area as ROI 7.
When plotting ROI, we
recommend using the slider below the image to move quickly
through the study to see if the desired structure (eg
gallbladder) due to movement in some phases of the dynam. the
study did not deviate from the plotted ROI.
The program creates curves of the time course of
radioactivity from the marked areas of interest and makes a
number of adjustments and corrections
:
The mathematical processing of these curves follows . At all stages of processing below, the program first asks if we want to execute them, and they are executed only if the answer is yes. This saves evaluation time in cases where we are only interested in some parameters, or only visual and qualitative data.
Analysis of liver perfusion
If a fast group of images capturing the perfusion phase has been recorded, liver perfusion can be (optionally) analyzed . The initial (ie perfusion) phase of the liver curve is displayed and it is possible to set the scale of the display in the horizontal direction (expansion-compression) for optimal presentation of perfusion dynamics. On the perfusion curves of the whole liver and parenchyma, the points of arrival of the radioindicator, the peak of the first bolus flow and the "valley" of the plate separating the perfusion and parenchymatous phases of the liver curve are automatically marked (with the possibility of manual correction) . For the whole liver and parenchyma, the index quantifying perfusion is calculated - Washid's perfusion-flow index , which, based on the ratio between the descending and ascending arms of the peak of the first bolus pass, quantifies the part of the blood-borne radio indicator that flows through the liver and continues through the bloodstream, in contrast to the second part that is filtered by the liver (analogous to Fig.3.4.1a) .
Quantification of excretion from liver curves
First, the curves of the whole liver, parenchyma and intrahepatic bile ducts are processed . The maximum points and the start and end point of the excretion quantification section are automatically defined on the curves (with the possibility of manual modification). This section is interpolated by the least squares method of exponential functions, similar to nephrographic curves. The fit graph is displayed and the maximum time and half-life are calculated .
Blood-pool curve processing and determination of total clearance
As with dynamic renal scintigraphy, mathematical analysis of the rate of decrease in the concentration of the hepatotropic radiolabel in the bloodstream can be used to determine the total clearance of the liver and, more precisely, the total clearance of the radiolabel from the blood pool. Under normal circumstances, this total clearance is due to liver function, but in pathological cases the kidneys may also contribute to it.
The time course of the concentration of the radiolabel in the bloodstream (from ROI1) has a typical shape similar to that of a dynamo. renal scintigraphy (Fig. 3.9.1): Immediately after application it reaches the maximum value almost by leaps and bounds, then the curve decreases relatively quickly, mainly due to the distribution of the radioindicator into the extracellular space. The rate of decline decreases until after about 40 minutes the steady monoexponential course is reached, given the clearance of the radioindicator from the bloodstream, mainly by the activity of the liver. The rate of this monoexponential decline is proportional to the global clearance of the radiolabel, i.e. essentially the functional fitness of the liver .
The start and end points for the fit of the multiexponential function are marked on the curve from the bloodstream (from ROI1). If we do not rely on automatic marking, we define the starting point of the fit shortly after the arrival of the activity in a place where the initially chaotic course of the curve has already stabilized on a monotonic descent; the end point of the fit is best defined at the end of the curve - about 60 minutes. Iterative procedure followed by the laying of multi-exponential function (same as the dynamos. Kidney - see kap.3.4) curve course of radioactivity in the bloodstream, while the display shows a graph fiting and value half-time of clearance . Next, the program asks if we want to calculate the global clearance of the radio indicator. The total clearance of the radioindicator is given by the product of the rate coefficient of the asymptotic exponential R5 and the distribution volume of the radioindicator V D : GFR = R5. V D . The value of R5 is calculated from the fitting of the blood-pool curve. To determine the value of the distribution volume of the radiopharmaceutical V D, we can again choose two methods in the program: calculation based on the value of applied activity and measured activity of the collected blood sample, or determination (resp. Estimate) of distribution volume by empirical formula from patient height and weight. In a manner analogous to dynamos. the value of the global clearance of the radioindicator in [ ml./sec. ]. The clearance results are displayed on a field display with color-coded bloodstream fitting curves.
Deconvolution analysis - calculation of transit functions and times
This is followed by an (optional) calculation of the transit functions and the transit times of the passage of the radioindicator through the whole liver and parenchyma. Transit functions are constructed in a manner analogous to dynamic renal scintigraphy (Chapter 3.4) using Laplace deconvolution of liver curves (corrected for tissue and intravascular background) with an interpolated exponential bloodstream curve, which is taken as the input function. The deconvolution- formed transit function represents a hypothetical liver curve that would arise, if the applied radioindicator would be injected as a bolus directly into the vascular system of the liver (hepatitis artery). The points of minimum, mean and maximum transit time are automatically defined on the transit curves (with the possibility of manual modification). After processing both transit curves of the whole liver and parenchyma, these curves are displayed together with the values of transit times, from which we can conclude the possible absolute and mutual extension of the transit of the radioindicator through the whole liver and parenchyma .
In a well-functioning hepatic parenchyma,
virtually 100% of the HIDA radiolabel is taken up and metabolized
in liver cells (hepatocytes) and transported by the intrahepatic
bile ducts as it first flows through the hepatic vascular bed. In
liver damage, this uptake is slowed down and the radiolabel
recirculates in the bloodstream for a longer period of time.
The hepatic extraction fraction (HEF) indicates
which part of the radioindicator is taken up in one pass through
the vascular bed of the liver parenchyma (or the remaining
untaken part passes through and recirculates in the bloodstream).
Thus, the hepatic extraction fraction quantifies the functional
capacity of the liver parenchyma . It is usually
expressed as a percentage, normal values are close to 100%
(90-100%), in severe liver damage they can be reduced to 10%.
The hepatic extraction fraction can be calculated by analyzing
the above transit function of the liver parenchyma, resulting
from the deconvolution of the parenchyma curve with the
bloodstream curve. This curve corresponds to the hypothetical
course of radioactivity in the liver, when the radioindicator is
applied directly into the blood supply of the liver (into the
artery hepatis). The transit curve of the parenchyma should
ideally have a 100% uptake, roughly a monoexponential course
(Fig. left) caused by the dilution excretion of the
radioindicator into the bile ducts. However, with a reduced
extraction fraction, the transit curve has a more complex course,
shown in Fig. on the right. At the beginning, there is a rapid
decrease, caused by the free passage of part of the radiolabel
further into the bloodstream, after which the curve continues
with a slower decrease reflecting the transport of the captured
radiolabel into the intrahepatic bile ducts. The size ratio of
the two components indicates the value of the hepatic HEF
extraction fraction.

Calculation of the hepatic extraction fraction HEP based on the
analysis of the deconvolution transit curve of the parenchyma.
The calculation is performed by interpolating
the monoexponential function EXP(t) = A.e-k.t through
the middle part of the transit curve TF of the liver parenchyma,
extrapolating to t ® 0 and calculating the ratio of the height of this
exponential at the minimum transit time TTmin to the total height of the transit function :
HEF = [EXP(TTmin) / TF(TTmin)]. 100 [%].
It should be noted that this calculation is usually only
approximate, as transit curves are often irregular in shape and
show statistical fluctuations.
Quantification of prominent images and curves of the bile ducts
Based on the quantitative analysis of the liver curves, the respective images are captured and images of the liver in the perfusion, secretion, early and late excretion phases are displayed, while the text of the visual evaluation of the images is offered for control and editing at the bottom of the screen.
This is followed by
processing of the curves of the gallbladder, d.choledochus,
interstitial tract and possibly stomach. For each of them, the moment
of arrival of the radioindicator is determined , the linear regression function is interpolated with an
ascending section (the fit graph is displayed) and the slope
of the
radioactivity increase in percent of liver activity per
hour is quantified (Fig. 3.10.1). In addition, an event time is
inserted for the gallbladder at the request of the program.
application of cholekinetics and optionally the
gallbladder ejection fraction is calculated(Fig.3.10.1). The
curves of the whole liver, parenchyma, d.choledochus,
gallbladder, interst are then displayed on the screen. tract and
event. stomach with a clearly marked vertical line indicating the
moment of cholekinetics application. The values of the calculated
dynamic parameters for these curves will also be displayed
(Fig.3.10.1) and in the lower part of the screen the text of the
verbal evaluation will be offered for editing, where we can
comment on the size and shape of cholescintigraphic curves.
gallbladder response to cholekinetikum, severity
event. duden-gastric
reflux, and the like .. The picture analysis biliary appropriate
(especially in pathological cases) as intermediate results print
documentation - obr.3.10.1:
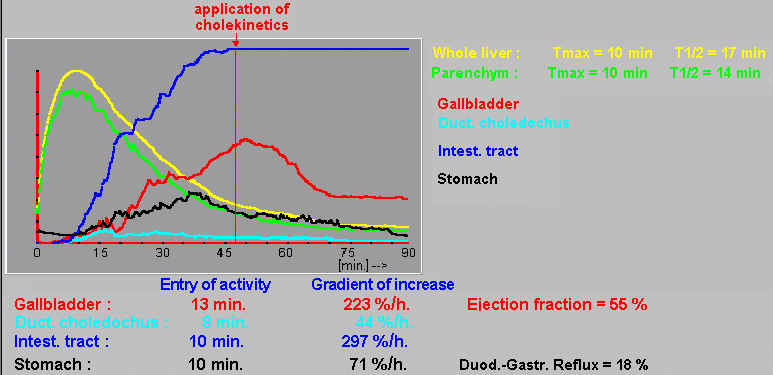
The resulting protocol
Finally, a summary image is displayed on the screen containing images of significant phases of the dynamic study (images of perfusion and secretion phases of the liver, early and late excretion phases to the intestinal tract), curves of liver, parenchyma, d.choleduch, gallbladder, intestinal tract and transit functions of whole liver and parenchyma. Below them is a re h ice kvantitativnícvh most important parameters calculated by the program. At the bottom of the screen, the word evaluation text is displayed, which can be modified and supplemented. The same is true of the text "Conclusion" if its standard wording has been generated; otherwise you xt the final evaluation will be entered here, including the signature of the doctor. Finally, a final report is printed (in the required number of copies) containing significant images, curves, calculated parameters and verbal evaluation, including the conclusion and signature of the doctor Fig.3.10.2:
| Department
of Nuclear Medicine, University
Hospital About diet
Date:
.............. Name of patient: ....................... . Birth
certificate number: .........................
|
|
| Mathematical analysis and complex evaluation of dynamic functional scintigraphy of the liver and bile ducts - cholescintigraphy | |
 |
|
| Evaluation:
After intravenous administration of the radioindicator,
the liver of the usual shape and size is imaged in a
timely manner. The liver parenchyma does not show focal
changes. Bile ducts can be differentiated from 10
minutes, from 13 minutes. the gallbladder begins to fill.
In 30.min. a cholekinetic stimulus was administered. In
the next course, we observe a rapid passage of the
radioindicator through the biliary system with a smooth
outflow through the ductus choledochus into the intest.
tract. Conclusion:
Visual evaluation of sequential images and quantitative
analysis of liver curves indicate good
hepatocellular function , rapid transit through
the liver parenchyma and free drainage of the biliary
system, without signs of biliary obstruction. The
gallbladder has a good filling and evacuation function. |
HEPDYN program structure
The HEPDYN program consists of the following parts:
HEPDYN 1 - display of a series of images, verbal evaluation, marking of ROI,
creating curves
HEPDYN 2 - mathematical processing of curves, quantification of clearance
HEPDYN 3 - deconvolution, calculation of transit functions and times
HEPDYN 4 - summation of images of secretory and excretory phase, verbal evaluation
HEPDYN 6 - displaying results, editing texts, printing a report
At the same time, this structure shows how to proceed when the calculation is interrupted or when the program is restarted in order to repeat a certain part of the calculations. E.g. to change the texts of the verbal evaluation, just run HEPDYN6, to repeat the calculation of the clearance parameters, run HEPDYN2 (after which we can omit HEPDYN3 and 4 and continue by running HEPDYN5).
Cast of SAVE and REA after the end of the HEPDYN program :
SA 1 - ROI, curves
SA 10 - image of perfusion phase
SA 11 - image of
secretory phase
SA 12 - image of early excretion phase
SA 11 - image of late excretion phase